Introduction
Drug-induced delayed cardiac repolarization, a recognized risk factor for pro-arrhythmia, is the single most common cause for the withdrawal of prescription drugs. The vast majority of drugs known to prolong the repolarization of the cardiac membrane preferentially inhibit the delayed rectifier current (I Kr) by binding to the hERG K+ channel. Consequently, functional in vitro assays for predicting a drug’s potential to delay cardiac repolarization typically include evaluating hERG K+ channel block in transgenic cell lines, or action potential duration assays with primary canine or rabbit Purkinje fibers. However, the predictive value of these existing assays is limited due to species differences and the lack of complex ion channel interactions in cell lines overexpressing the hERG K+ channel.1 Improved simulation of cardiac networks could allow for drug discovery stage testing to elucidate off-target effects, including detrimental hERG K+ channel interactions. This ability will improve drug safety screening and reduce the cost and time of drug development.
A compelling approach to this issue uses assays performed on human embryonic stem cell-derived (hESC) cardiomyocytes. Cytiva Plus Cardiomyocytes are hESC-derived and exhibit the morphology and electrophysiological activity typical of human cardiomyocytes, while the Axion BioSystems Maestro Microelectrode Array (MEA) system provides a high throughput platform for the evaluation of extracellular field potentials. Combining these two technologies creates a robust platform for cardiotoxicity profiling.
Materials and Methods
To induce a cardiomyocyte phenotype, hESCs (H7 cell line) were subjected to a controlled differentiation process. Briefly, the hESCs were adapted to alternative growth conditions, subjected to growth factor induction, followed by a period of cardiomyocyte maturation. At the end point of differentiation, cardiomyocytes were harvested and cryo-preserved at 1x106 cardiomyocytes per vial.
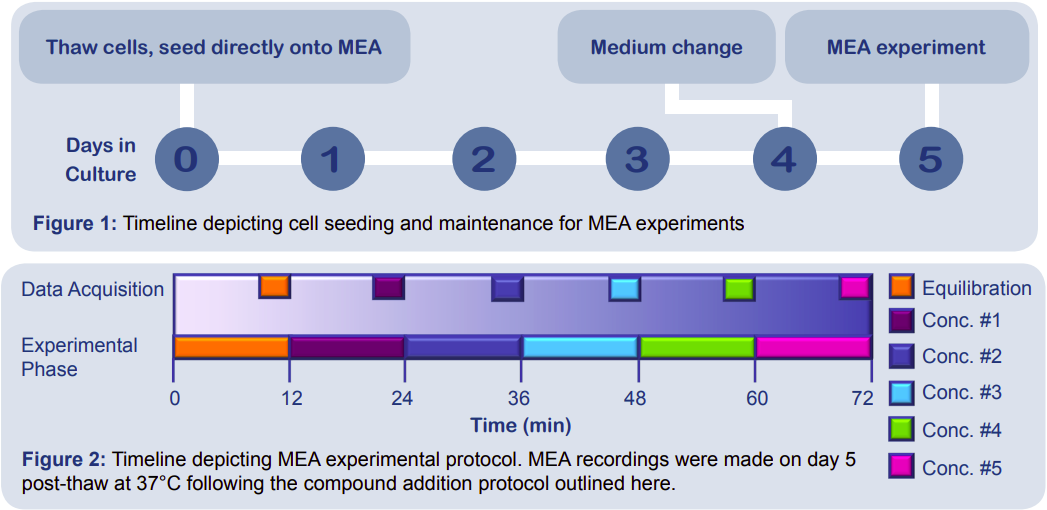
Following the timeline presented in Figure 1, Cytiva Plus Cardiomyocytes (GE Healthcare) were seeded directly from thaw onto multiwell MEA plates (Axion BioSystems) at a density of 60,000 cells in a 4 μL dot over the electrode array using the optimized culture protocol. On day 4 post-thaw, half of the seeding medium was replaced with fresh medium. Treatment of the cells on the MEA on day 5 postthaw followed the timeline outlined in Figure 2. For a step-by-step guide on the culture methods, please review the Full Culture Protocol.
Results
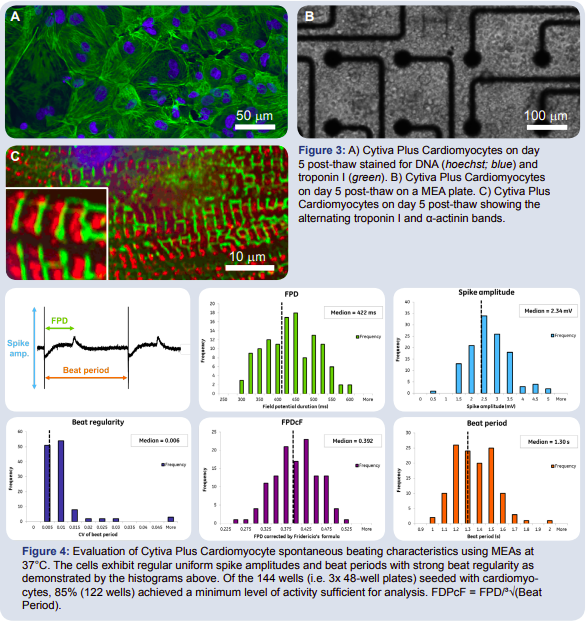
To characterize the Cytiva Plus Cardiomyocytes, the cells were stained on day 5 post-thaw for DNA (hoescht stain, blue) and troponin I (green), a protein critical for skeletal and cardiac muscle contraction (Fig. 3). The contractile nature of the cells was confirmed by the prevalence of troponin I. When grown on an MEA plate (Fig. 3), the cardiomyocytes formed a uniform monolayer on top of the microelectrode array. This conformation produced a functional syncytium of cells with a robust electrophysiological signature. The Maestro MEA system was used to record spike amplitude and timing of the field potential, allowing for calculation of beat period, beat regularity, field potential duration (FPD) and field potential duration corrected by Fridericia’s formula (FPDcF).
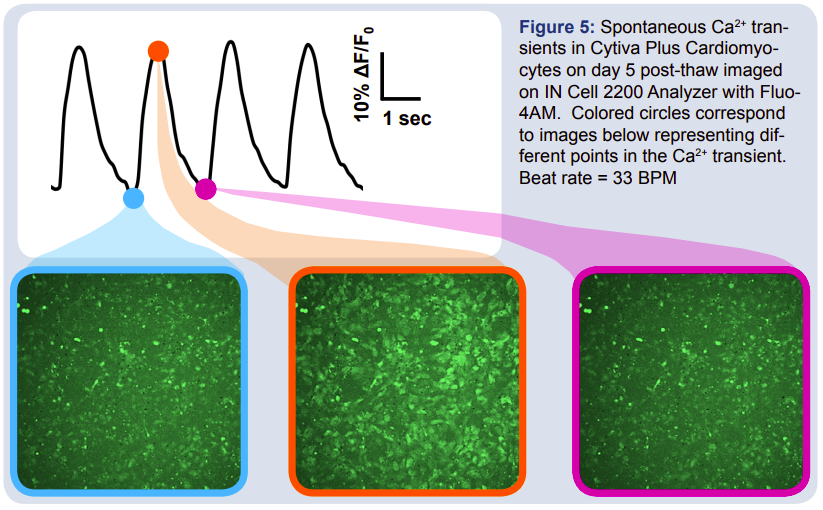
To establish baseline parameters for the Cytiva Plus Cardiomyocytes, an MEA was plated according to the Cytiva Plus Protocol, and the spontaneous beat characteristics were evaluated. Figure 4 shows histograms of the median measures for spike amplitude, beat period, beat regularity, and two measures of field potential duration. The data show well-defined spontaneous beat regularity between cultures. In order to verify the beating of the cardiomyocytes, a Fluo-4AM dye was used to stain for calcium (Ca2+) transients that occur during spontaneous cardiac beating. The beat rate of the cells can be determined by assessing the change in fluorescence over time as depicted in Figure 5. The blue and magenta images demonstrate the Ca2+ concentration before initial depolarization of the cardiomyocytes. The orange image shows the cells following the initial depolarization of the action potential, when the calcium influx produces the plateau phase of the cardiac action potential.
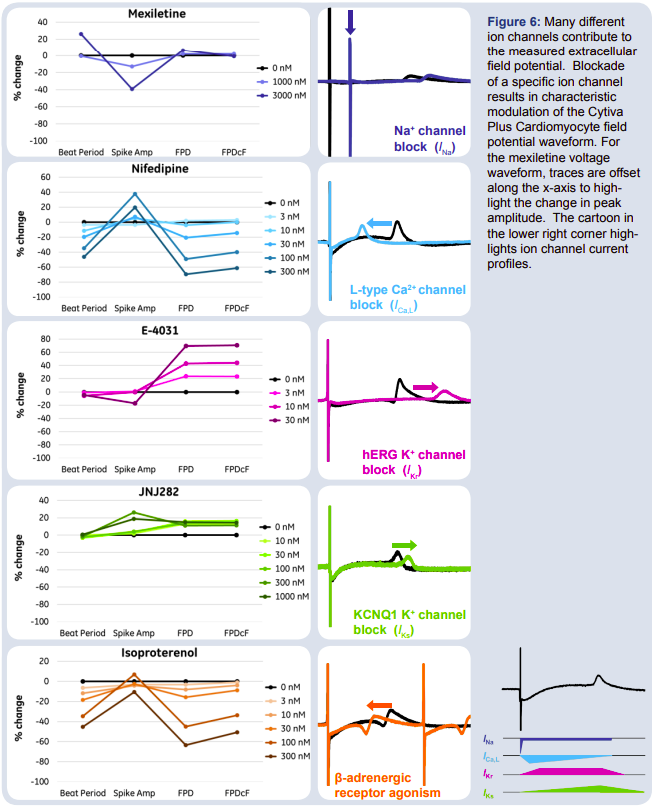
In order to evaluate the modulation of the Cytiva Plus Cardiomyocyte field potentials, specific ion channels were pharmacologically manipulated with the compounds described below. Results are summarized in Figure 6.
- Mexiletine (INa): Sodium channel blocker that reduces the spike amplitude by affecting the depolarization phase of the cardiac action potential. This compound blocks sodium channels with fast association/dissociation kinetics.
- Nifedipine (I Ca,L): L-type calcium channel blocker that causes the repolarization phase of the cardiac action potential to occur earlier by stabilizing voltage gated L-type Ca2+ channels in their inactive conformation.
- E-4031 (I Kr): hERG potassium channel blocker (fast current channels) that delays the repolarization phase and results in an extended FPD, leading to arrhythmias.
- JNJ282 (I Ks): Slow potassium channel blocker, which affects the KCNQ1 K+ channel yielding similar, but smaller FPD prolongation as compared E4031.
- Isoproterenol (ADR-β1): A β-adrenergic agonist (similar to adrenaline) leading to increased beat rate and shorter FPDs.2
The Cytiva Plus Cardiomyocytes exhibited the expected electrophysiological phenotypes in response to pharmacological manipulation with these selective ion channel modulators.
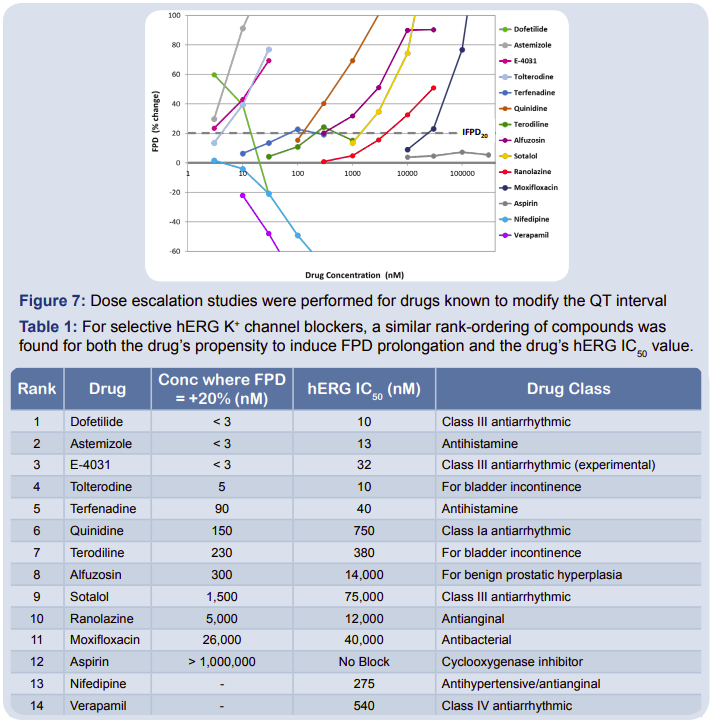
When combined with MEAs, the Cytiva Plus Cardiomyocytes serve as a model system for evaluating cardioactive compounds. To validate Cytiva Plus Cardiomyocytes as a potentially useful new in vitro test system for drug-induced delayed cardiac repolarization, multiple drugs were applied to the cardiomyocytes to determine their effect on the FPD (Fig. 7). Drugs that triggered a 20% or greater prolongation of the FPD were compiled and ranked based on the concentration required to elicit the FPD change. A positive relationship was found between this concentration and the hERG IC50 values across all drug classes (Table 1).
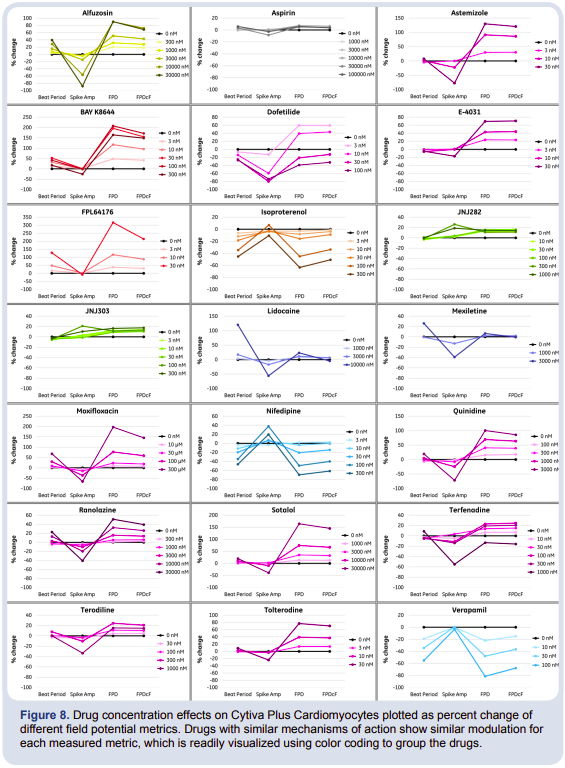
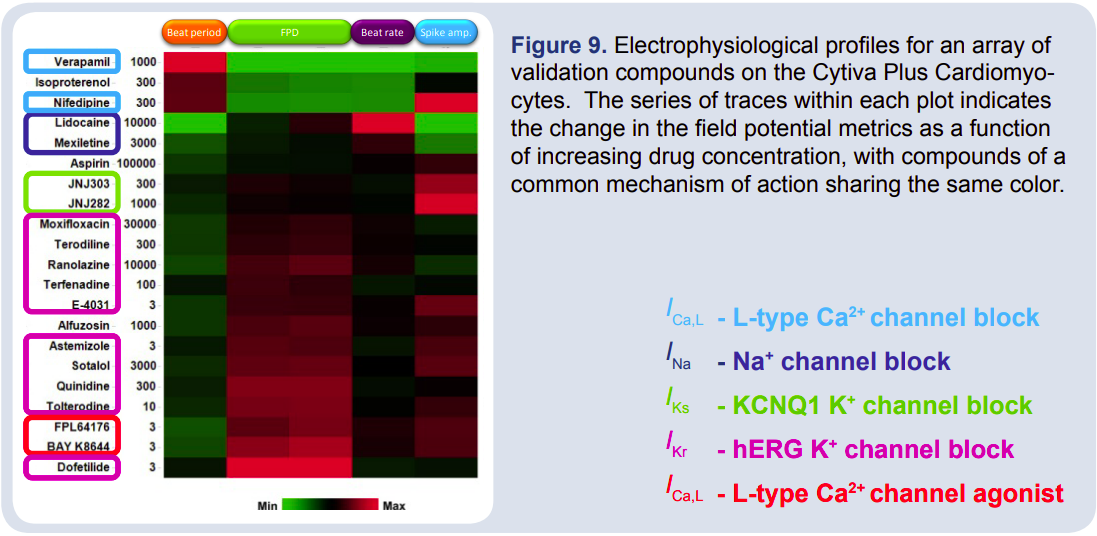
In combination with the field potential duration, the beat rate and spike amplitude of the field potential waveform establishes the electrophysiological profile of cardioactive compounds, as depicted in Figure 8, and provides information on the mechanism of action. For example, while hERG blockers Sotalol and Ranolazine have 2 different clinical uses, both show similar modulation of field potential metrics: increased beat period, prolongation of the FPD, and decreased spike amplitude. A hierarchical clustering analysis was performed on these electrophysiological profiles (Figure 9). Compounds acting through similar mechanisms clustered together, suggesting that application of these metrics to unknown or novel drugs could be used to predict mechanism of action.
Conclusion
Cytiva Plus Cardiomyocytes are hESC-derived cardiomyocytes that exhibit morphology and electrophysiological responses consistent with human cells. The cultured cells form spontaneously beating monolayers whose extracellular field potential characteristics can be readily examined using Axion BioSystems MEAs.
Together, the Cytiva Plus Cardiomyocytes and Maestro MEA system offer an in vitro system for evaluating the electrophysiological effects of cardioactive compounds. The field potential waveform was sensitive to selective manipulations of multiple ion channels contributing to the cardiac action potential, including the hERG potassium channel. Notably, there was a positive relationship between the IC50 values of hERG channel blockers and the concentration that elicited a 20% increase in FPD. Extension of the analysis to include multiple field potential metrics allowed the development of electrophysiological profiles of known cardioactive compounds. Compounds with shared mechanisms of action displayed quantitatively similar profiles in a hierarchical clustering analysis, providing support for mechanism prediction for novel pharmaceuticals.1
Based on these results, an MEA assay using hESC-derived cardiomyocytes could complement or replace a portion of the pre-clinical cardiac toxicity screening tests currently used for lead optimization and further development of new drugs.
References
1. Clements & Thomas, High-Throughput Multi-Parameter Profiling of Electrophysiological Drug Effects in Human Embryonic Stem Cell Derived Cardiomyocytes using Multi-Electrode Arrays. Toxicol Sci, 2014
2. Grant, A.O., Cardiac ion channels. Circ Arrhythm Electrophysiol, 2009. 2: p. 185-94.



